Regular screening is one of the most important ways to prevent colorectal cancer (colon and rectal).
“Colorectal cancer is the third-leading cause of cancer death in the U.S. And we expect about 50,000 people will die this year from colorectal cancer,” Dr. Lisa Boardman, a Mayo Clinic gastroenterologist.
Everyone at age 45 is recommended to begin regular screening. The U.S. Preventive Services Task Force updated its guidelines in 2021 to include starting screening five years earlier than the previous recommendation of 50, after studies showed increased rates of cancer in younger people.
“What we’re seeing now is more people developing colorectal cancer under the age of 50. In fact, 10% of colorectal cancer cases now are going to occur in people who are under the age of 50,” says Dr. Boardman.
Those at higher risk include African Americans, those with a family history of colorectal cancer and who have other health issues, including diabetes. It’s important to talk with your health care team to determine when to begin screening.
Watch: Dr. Lisa Boardman discusses colorectal cancer.
The goal for colorectal cancer screening is to check for signs of abnormal cells in the colon or rectum, and treat them before they become cancerous.
There are multiple types of screening options, but colonoscopy is the most common screening test.

During a colonoscopy, a long, flexible tube, called a colonoscope, is inserted into the rectum. A tiny video camera at the tip of the tube allows your health care professional to detect changes or abnormalities inside the entire colon.
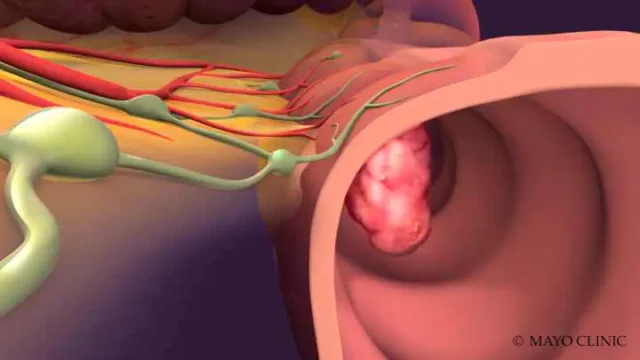
Your health care professional may remove a polyp during a colonoscopy. Not all colon polyps develop into cancer, but most colon cancers begin as polyps.
Types of screening and recommended intervals include:
- Fecal immunochemical test (FIT), annually.
- High-sensitivity guaiac-based fecal occult blood test (HSgFOBT), annually.
- Multitarget stool DNA (MT-sDNA) test, every three years.
- Colonoscopy, every 10 years.
- CT colonography (CTC), every five years.
- Flexible sigmoidoscopy (FS), every five years.
How long you should continue regular colorectal cancer screening will depend on your age and results of your screenings. It’s important to work with your health care team to determine what screening option is best for your individual risk factors.
These lifestyle changes also can play a role in reducing risks for colorectal cancer:
- Eat a low-fat, high-fight diet.
- Get regular exercise.
- Don’t smoke.
- Consume alcohol in moderation.
- Maintain a healthy weight.
Learn more about colorectal cancer at the Mayo Clinic Comprehensive Cancer Blog.
Related stories:
- Mayo Clinic researchers study rare genetic condition to tackle colorectal cancer
- Mayo Clinic Q and A: Colorectal cancer screening remains important.
- Mayo Clinic Minute: Symptoms of colorectal cancer.
The post Can colorectal cancer be prevented? appeared first on Mayo Clinic News Network.
“Courtesy: Lisa Boardman, M.D/Gastroenterology/Mayo Clinic.”
Republished with permission[/vc_message]
Disclaimer
Artificial Intelligence Disclosure & Legal Disclaimer
AI Content Policy.
To provide our readers with timely and comprehensive coverage, South Florida Reporter uses artificial intelligence (AI) to assist in producing certain articles and visual content.
Articles: AI may be used to assist in research, structural drafting, or data analysis. All AI-assisted text is reviewed and edited by our team to ensure accuracy and adherence to our editorial standards.
Images: Any imagery generated or significantly altered by AI is clearly marked with a disclaimer or watermark to distinguish it from traditional photography or editorial illustrations.
General Disclaimer
The information contained in South Florida Reporter is for general information purposes only.
South Florida Reporter assumes no responsibility for errors or omissions in the contents of the Service. In no event shall South Florida Reporter be liable for any special, direct, indirect, consequential, or incidental damages or any damages whatsoever, whether in an action of contract, negligence or other tort, arising out of or in connection with the use of the Service or the contents of the Service.
The Company reserves the right to make additions, deletions, or modifications to the contents of the Service at any time without prior notice. The Company does not warrant that the Service is free of viruses or other harmful components.












