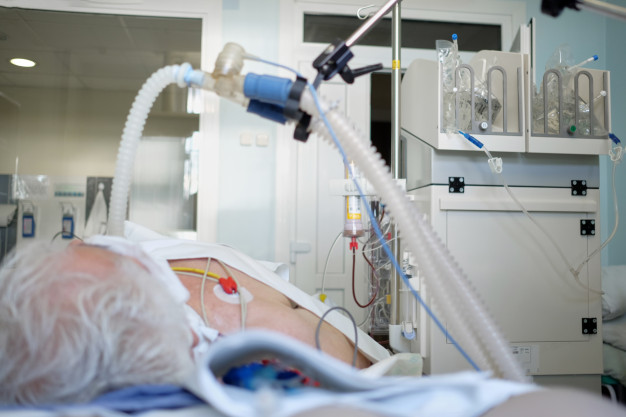
People with certain underlying health conditions, such as diabetes, are at greater risk of severe illness from COVID-19. And now it appears that there also may be a relationship between severe COVID-19 infections and new cases of diabetes.
Preliminary studies found that more than 14% of patients who were hospitalized with COVID-19 and recovered also were newly diagnosed with Type 1 or Type 2 diabetes. It’s something that medical experts are watching closely.
“So when the immune system is not working as well and tends to work against the insulin-making cells, even when the sugar is normal, you can diagnose this with certain tests, such as antibody tests. And if in such individuals there is an illness, that can worsen the sugar in these people. So that could be an explanation for why Type 1 diabetes might be diagnosed after COVID-19 — that these are individuals who were already predisposed,” says Dr. Yogish Kudva, a Mayo Clinic endocrinologist whose clinical focus is diabetes.
Researchers say it’s not clear yet if diabetes directly results from severe COVID-19 illness. And in the case of Type 2 diabetes, the virus could be quickening the development of the disease for those with existing risk factors, such as prediabetes, obesity and high blood pressure.
“This individual is predisposed to abnormal glucose characteristics, abnormal glucose regulation, and then severe COVID happens. That’s going to accelerate the progression from this state toward a more uncontrolled state,” says Dr. Kudva.
He says there is still much to be learned about the long-term effects of COVID-19, but it is clear that people with diabetes are at higher risk for developing severe illness from the virus.
“It appears now that people with diabetes seem to develop more severe COVID-19 disease. It’s not that people with diabetes are more prone to COVID-19. But if they develop COVID-19, the disease is much more severe and seems to progress quicker. That seems to happen both with Type 2 and Type 1 diabetes,” says Dr. Kudva.
He says it’s important to immediately begin improving underlying health conditions that may cause diabetes and follow COVID-19 safety precautions.
“Rigorous attention to all the primary preventive measures that we use: mask-wearing, social distancing, hand-washing — I think those things continue to be relevant and will continue to be relevant for quite some time yet. We are still in the middle of the pandemic,” says Dr. Kudva. “I think a second issue would be physical fitness. Doing whatever they can, given the limitations that we have, making sure that they adhere to all the guidelines of what to do safely indoors and outdoors. And, therefore, work on improving physical fitness. Clearly, physical activity is an important component of every day and adds to our fitness and therefore our ability to withstand every severe illness. So that’s the second component. And then the third component would be if they do fall sick, to seek attention early. And then the fourth component is the vaccine.”
‘Courtesy: Yogish Kudva, M.B.B.S. / Endocrinology / Mayo Clinic.’[/vc_message]
Disclaimer
Artificial Intelligence Disclosure & Legal Disclaimer
AI Content Policy.
To provide our readers with timely and comprehensive coverage, South Florida Reporter uses artificial intelligence (AI) to assist in producing certain articles and visual content.
Articles: AI may be used to assist in research, structural drafting, or data analysis. All AI-assisted text is reviewed and edited by our team to ensure accuracy and adherence to our editorial standards.
Images: Any imagery generated or significantly altered by AI is clearly marked with a disclaimer or watermark to distinguish it from traditional photography or editorial illustrations.
General Disclaimer
The information contained in South Florida Reporter is for general information purposes only.
South Florida Reporter assumes no responsibility for errors or omissions in the contents of the Service. In no event shall South Florida Reporter be liable for any special, direct, indirect, consequential, or incidental damages or any damages whatsoever, whether in an action of contract, negligence or other tort, arising out of or in connection with the use of the Service or the contents of the Service.
The Company reserves the right to make additions, deletions, or modifications to the contents of the Service at any time without prior notice. The Company does not warrant that the Service is free of viruses or other harmful components.